Many of us, or someone we know, has diabetes. But why are most patients on daily medication, while some have to use insulin shots daily?
It’s because there are basically two types of diabetes, type 1 and type 2. These are two distinct conditions with very different causes, onset patterns, and management approaches.
Knowing the difference in type 1 and type 2 diabetes is not just a matter of medical curiosity. It directly shapes how a person lives, treats, and understands their condition.
What Is Diabetes, at Its Core?
At its simplest, diabetes is a condition where the body struggles to manage blood sugar levels. The hormone responsible for allowing blood sugar to enter cells is insulin, which is produced by the pancreas.
When insulin production stops or doesn’t work properly, blood sugar builds up. That is where type 1 and type 2 diverge significantly.
| Shocking Fact! 589 million adults worldwide are currently living with diabetes, accounting for 1 in every 9 adults globally. |
Type 1 Diabetes: When the Immune System Turns Against Itself
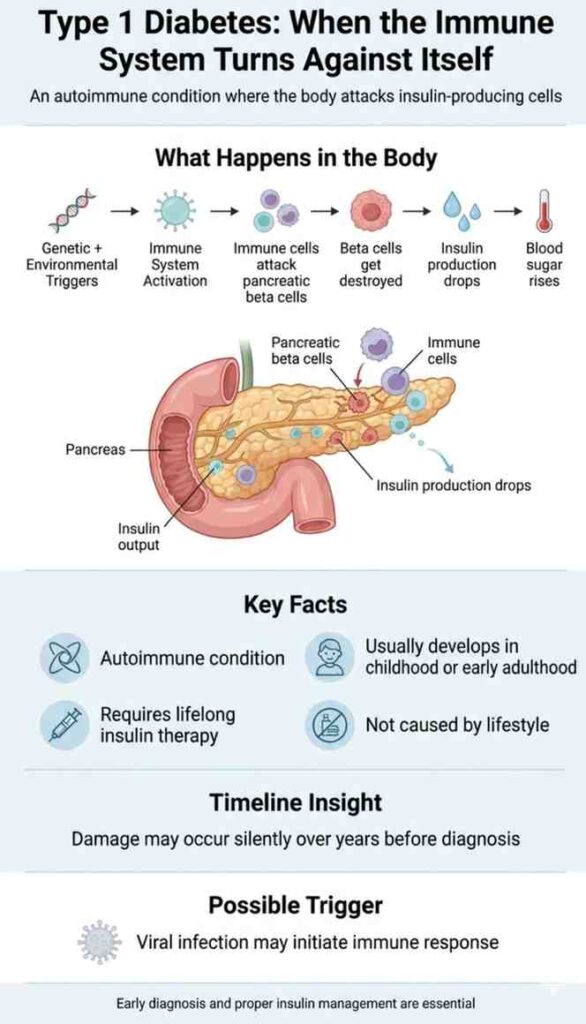
Type 1 diabetes is a progressive autoimmune disease. Meaning the immune system makes a serious mistake. It identifies the insulin-producing cells as a threat and destroys them.
This is what happens:
- Your body’s immune system (which usually protects you) sometimes gets confused because of a mix of genes (what you’re born with) and environmental triggers (like infections)
- Because of this confusion, the immune system attacks the beta cells in the pancreas
- As more and more beta cells are damaged, the body can’t produce enough insulin, leading to very low or no insulin levels.
- This damage doesn’t happen overnight; it can take years before symptoms appear and diabetes is diagnosed.
- One possible trigger for this immune attack is a viral infection, which may start the whole process in some people.
Because the pancreas can no longer produce insulin, people with type 1 diabetes need external insulin every day to survive. There is currently no way to prevent it through lifestyle changes.
Type 1 diabetes affects approximately 1% of the population. While it is often diagnosed in childhood or young adulthood, it can appear at any age.
Type 2 Diabetes: When the Body Stops Listening to Insulin
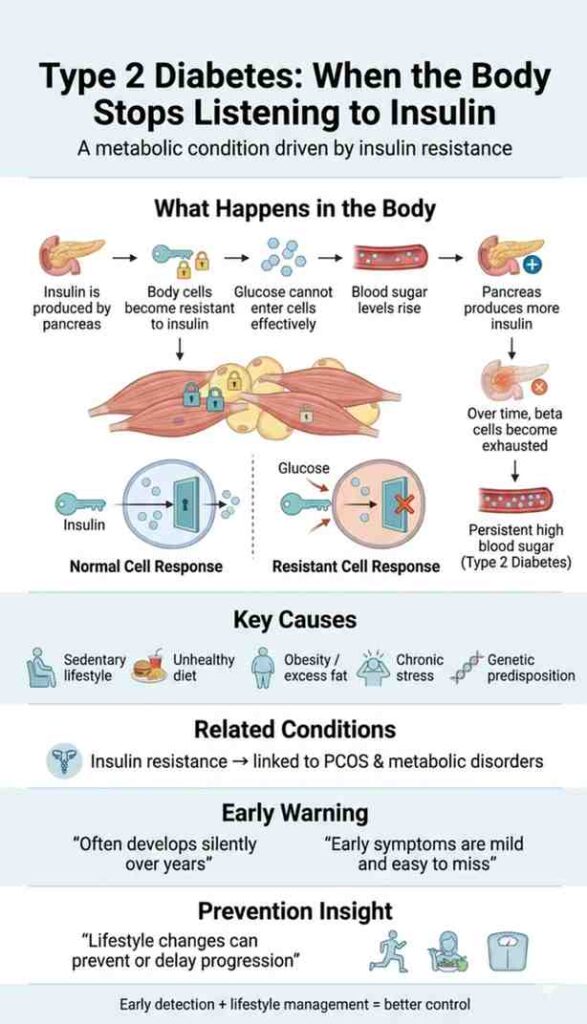
Type 2 diabetes works differently. Here, the pancreas still produces insulin, but the body’s cells do not respond to it effectively. It’s less about a lack of insulin and more about the body ignoring it.
Here’s what actually happens:
- Insulin is still being produced. Your pancreas continues to make insulin.
- But the body becomes resistant. Cells in muscles, liver, and fat stop responding properly to insulin; this is called insulin resistance.
- Sugar starts building up in the blood. Since cells aren’t “listening,” glucose can’t enter them efficiently, leading to high blood sugar levels.
- The pancreas tries to compensate. It produces more insulin to overcome this resistance.
- Eventually, the system gets exhausted. Over time, pancreatic beta cells can’t keep up with the high demand, resulting in persistent high blood sugar (hyperglycemia).
Why does this happen?
Lifestyle factors strongly influence type 2 diabetes:
- Sedentary routine (long sitting hours)
- Unhealthy diet (high sugar, processed foods)
- Obesity or excess body fat
- Chronic stress
- Urban lifestyle habits
This is why early lifestyle intervention is effective in preventing and managing type 2 diabetes. In fact, understanding and addressing prediabetes at the right time can help reverse or delay the progression of the condition.
Insulin resistance doesn’t stop here. It can quietly impact other parts of your health, too. It is closely linked to conditions like PCOS (Polycystic Ovary Syndrome).
Unlike type 1, type 2 is strongly associated with lifestyle choices, though genetics still plays a role. It develops gradually and often goes unnoticed for years. Research is ongoing in different parts of the world to find a cure for type 2 diabetes, and some approaches have already shown promising results.
Type 2 diabetes affects approximately 8.5% of the adult population worldwide.
The Key Differences at a Glance
Both types affect blood sugar, but they do so through entirely different mechanisms. Here is a side-by-side look at how they compare across the factors that matter most.
| Factor | Type 1 Diabetes | Type 2 Diabetes |
| Cause | Autoimmune destruction of beta cells | Insulin resistance and beta cell exhaustion |
| Insulin Production | Little to no | Present, but used ineffectively |
| Age of Onset | Often childhood or young adulthood | Usually adulthood, increasingly in younger people |
| Onset Speed | Sudden and noticeable | Gradual, often silent for years |
| Genetic Link | Weaker genetic association | Stronger genetic association |
| Lifestyle Influence | Not caused by lifestyle | Strongly linked to diet, activity, and weight |
| Primary Treatment | Insulin therapy (lifelong) | Lifestyle changes, oral medications, or insulin |
| Preventable | No | Largely yes, with early intervention |
Understanding the Difference Is the First Step
Type 1 and type 2 diabetes are not the same condition wearing the same label. One is an autoimmune disorder requiring lifelong insulin; the other is a lifestyle-influenced disease that can often be delayed or managed with the right habits. Understanding this difference helps you seek the right care, make informed lifestyle choices, and approach diabetes with both clarity and confidence.
If you are concerned about your blood sugar levels or have a family history of diabetes, it’s important to stay alert to the early symptoms of type 2 diabetes and speak with a healthcare professional. Early awareness is always the first step toward better health.
FAQs
Type 2 diabetes can go into remission with significant weight loss, a balanced low-calorie diet, and regular physical activity. Blood sugar levels may return to a normal range without medication. However, it requires consistent lifestyle modifications and regular monitoring to stay in remission. Consult with your doctor.
In type 1 diabetes, the immune system destroys insulin-producing beta cells completely. Since the body produces zero insulin, external insulin injections are the only way to keep blood sugar levels stable and prevent life-threatening complications.
No. There is no clinical evidence that Ayurveda can cure either type of diabetes. Certain herbs may support blood sugar management as a complementary approach, but they should never replace prescribed medical treatment or insulin therapy.
Both share symptoms like frequent urination, excessive thirst, and fatigue. The key difference is speed. Type 1 symptoms appear suddenly and intensely, while type 2 symptoms develop slowly and often go unnoticed for years.
References
- https://pubmed.ncbi.nlm.nih.gov/2221810
- https://pmc.ncbi.nlm.nih.gov/articles/PMC10574155/
- https://diabetesatlas.org/


Post Comment